To reposition a bedbound senior and prevent sores, you should regularly turn and shift their position every two hours, using gentle techniques with supportive tools like slide sheets or cushions. Make sure to elevate high-pressure areas such as heels, hips, and sacrum with proper padding, and utilize support surfaces that distribute pressure evenly. Keep the skin clean, check for redness, and adjust your approach if needed. Explore more tips to ensure their comfort and skin health.
Key Takeaways
- Reposition the senior every 2 hours, using smooth, coordinated movements to reduce shear and friction.
- Use proper support surfaces and padding, such as foam wedges or rolled towels, to offload pressure points.
- Employ gentle lifting techniques with slide sheets to prevent skin trauma during turning.
- Regularly check high-risk areas like sacrum and heels for redness, swelling, or skin changes.
- Communicate clearly with the resident, ensuring comfort and explaining each repositioning step.

SelectSoma Double-Thick Gel Seat Cushion for Long Sitting Pressure Relief for Back, Sciatica, Coccyx, Tailbone Pain – Cushion for Office Chair, Wheelchair, Car & Truck, Patio Chairs – Egg Seat Pad
DOUBLE-THICK SUPPORT & COMFORT: High-grade, double-thick honeycomb gel cushion provides superior pressure-relieving support and stays soft on pressure…
As an affiliate, we earn on qualifying purchases.
As an affiliate, we earn on qualifying purchases.
Understanding the Importance of Repositioning

Repositioning is essential for preventing pressure ulcers and maintaining your loved one’s skin integrity. When you shift their position regularly, you reduce the continuous pressure on vulnerable areas like the sacrum, heels, and hips. This helps improve blood flow and prevents tissue ischemia, which can lead to open sores. It also helps distribute body weight evenly, reducing shear and friction that damage the skin. Repositioning isn’t just about comfort; it’s a crucial part of skin preservation and overall health. Proper color accuracy in repositioning ensures that skin assessments are accurate and consistent, aiding in early detection of potential issues. Additionally, using advanced repositioning techniques can further reduce the risk of skin breakdown. Incorporating pressure redistribution strategies can significantly enhance skin protection. Being aware of proper body alignment can further optimize the benefits of repositioning. Regularly consulting with healthcare professionals about individualized repositioning plans can ensure the best outcomes for your loved one. By staying proactive, you protect your loved one from painful, costly complications, and promote healing and well-being. Proper repositioning is a simple yet essential step in thorough care for bedbound seniors.

YHK Tubular Slide Sheet Transfer, Car Transfer Aid Easy Slide Sheet Positioning for Automotive Bed Flip Repositioning Home Care Assisted Mobility for Elderly Device (Blue, 28"x47")
Material: YHK's tubular slip sheet adopts ultra-low friction polyester fabric, the fabric is very soft, the patient contact…
As an affiliate, we earn on qualifying purchases.
As an affiliate, we earn on qualifying purchases.
Establishing a Repositioning Schedule

Creating a consistent repositioning schedule is crucial for preventing pressure ulcers and maintaining your loved one’s skin health. By sticking to a routine, you guarantee no area bears prolonged pressure. To make this manageable, follow these steps:
- Reposition every 2 hours to relieve pressure and promote circulation.
- Check skin condition during each turn, adjusting timing if redness or damage appears.
- Use a visual or written schedule to stay organized and remind yourself of the plan.
- Remember that skin integrity is vital for overall health, and attentive repositioning supports this goal.
Consistency helps prevent sore development and reduces discomfort. Remember, early adjustments based on your loved one’s skin response can make a difference. Establishing and sticking to this routine is a vital part of their care, ensuring they stay comfortable and healthy.

Bedsore Turning Wedge Pillow Side Sleeping Body Positioning Anti Bed Sores Treatment Bedridden Elderly Patient Foam Cushion Prevent Pressure Ulcer Incline Wedge Medical Nursing Care After Surgery
【Innovative Design】Hollow out in the middle of the Bedsore turning wedge enhances air flow and avoids direct contact…
As an affiliate, we earn on qualifying purchases.
As an affiliate, we earn on qualifying purchases.
Proper Techniques for Turning and Moving

When turning a bedbound senior, always use safe techniques to safeguard their skin and prevent injury. Keep your body aligned and use proper body mechanics to reduce strain on your back and shoulders. Remember to communicate clearly with the resident to ensure comfort and coordinate movement smoothly. Incorporating connected devices can also help monitor skin integrity and alert caregivers to potential pressure points. Utilizing pressure ulcer prevention strategies can further support skin health during repositioning. Additionally, regularly assessing the resident’s skin condition can help identify early signs of pressure damage and prompt timely interventions. Using technological tools can enhance your ability to track and respond to skin changes more effectively. Employing pressure redistribution surfaces like specialized mattresses or cushions can also significantly decrease the risk of pressure sores during repositioning.
Safe Turning Methods
Proper turning and moving techniques are essential to protect fragile skin and prevent injuries during repositioning. To do this safely, follow these steps:
- Use a draw sheet or slide sheet to gently lift and turn the resident, reducing shear on the skin.
- Maintain smooth, coordinated movements with minimal friction, avoiding abrupt pulls or jerks.
- Communicate clearly with the resident, encouraging relaxation to ease movement and reduce discomfort.
- Utilizing specialized tools and techniques, such as foam wedges or turning boards, can further facilitate safe repositioning and decrease the risk of pressure injuries.
- Regularly check for pressure points after repositioning, ensuring offloading of bony areas. Keep the bed at a comfortable height for you, and avoid twisting your body. Using proper tools like pillows or foam wedges can help maintain position and prevent unnecessary strain. Being aware of infection control practices helps prevent skin infections and complications. Incorporating proper body mechanics when repositioning minimizes caregiver strain and enhances safety. Additionally, ensuring the resident’s skin remains dry and clean is vital for skin integrity, which can be compromised by moisture or friction. Safety and gentle handling are key to preventing skin injuries and ensuring comfort.
Using Proper Body Mechanics
Using proper body mechanics during turning and moving is essential to protect both you and the resident from injury. Start by positioning yourself close to the resident to minimize strain. Keep your back straight, bend at your hips and knees, and use your leg muscles to lift or pivot. Use smooth, coordinated movements rather than jerking or twisting. Engage your core to maintain stability. Always communicate with the resident to ensure they’re ready and comfortable. When turning, use the “scoop” technique with sheets to avoid skin shear. Keep the resident’s body aligned and avoid excessive pulling. Being aware of skin integrity and how to prevent pressure sores is crucial in repositioning. Understanding pressure redistribution techniques can further help prevent skin trauma. Applying proper repositioning methods consistently can also significantly reduce the risk of pressure ulcers. Incorporating pressure relief positions is vital for effective pressure sore prevention. Using these techniques reduces your risk of injury and helps prevent skin trauma, ensuring safe, effective repositioning. Additionally, being familiar with pressure management strategies can enhance patient comfort and safety during repositioning procedures.

Alcedo Alternating Air Pressure Mattress Pad for Bed Sore and Ulcer Prevention, Hospital & Home Use Medical Mattress Topper for Bedridden Patient, Adjustable Ultra Quiet Pump and Waterproof Cushion
Effective Bedsore Prevention with Medical-Grade Quality — With advanced alternating pressure technology, this mattress helps prevent and treat…
As an affiliate, we earn on qualifying purchases.
As an affiliate, we earn on qualifying purchases.
Selecting and Using Support Surfaces and Padding

When selecting cushions and padding, you need to prioritize support surfaces that distribute pressure evenly and safeguard vulnerable areas. Proper placement of padding, like foam wedges or rolled towels, helps offload bony prominences and prevent sores. Using the right support tools ensures comfort, reduces shear risks, and promotes safe repositioning. Incorporating adaptive lighting can also help caregivers and seniors better monitor skin integrity and identify early signs of pressure damage. Additionally, choosing support surface materials that are durable and breathable can further enhance comfort and skin health. Selecting materials with appropriate pressure redistribution properties can significantly improve outcomes for bedbound seniors, especially when combined with an understanding of auditory processing to better interpret sensory cues and discomfort signals.
Choosing Appropriate Cushions
Selecting the right cushions is essential for preventing pressure injuries and ensuring comfort for bedbound seniors. The right support surfaces can evenly distribute pressure and reduce shear. Here’s what to consider:
- Choose cushions made of memory foam or gel-filled materials to contour to the body and decrease pressure points.
- Use heel protectors or specialized heel cushions to prevent heel ulcers, especially when heels are suspended.
- Opt for alternating pressure cushions or mattresses to regularly shift pressure and enhance circulation.
Ensure cushions fit properly and are placed securely to avoid bunching or slipping. Regularly check for signs of redness or skin breakdown. Proper cushioning supports skin integrity, improves comfort, and reduces the risk of sores during repositioning.
Proper Padding Placement
Proper padding placement is essential for safeguarding pressure points and maintaining comfort during repositioning. You should select support surfaces like pillows, foam wedges, and rolled towels to offload areas prone to pressure, such as heels, sacrum, hips, elbows, and shoulders. Position these supports strategically to elevate bony prominences and prevent friction or shear forces. Confirm padding is snug but not too tight, avoiding folds or creases that could create new pressure points. When placing padding, verify it’s secure and stable to prevent shifting during movement. Using specialized cushions or heel protectors can further reduce pressure on vulnerable areas. Always check that the support surfaces are clean, dry, and properly positioned to promote circulation and minimize the risk of skin breakdown.
Positioning Strategies to Minimize Pressure

Effective positioning strategies are essential to minimize pressure and prevent skin breakdown in bedbound seniors. You want to avoid prolonged pressure on any one area, so regularly changing positions is key. Here are three effective methods:
Regular repositioning with proper support prevents skin breakdown in bedbound seniors.
- Use the 30-degree lateral tilt position instead of full side-lying to reduce sacrum and trochanter pressure while maintaining stability.
- Elevate the head 30-45 degrees in a semi-recumbent position to redistribute pressure and promote breathing.
- Avoid staying in one position longer than two hours; instead, rotate through supine, side-lying, and semi-recumbent positions to prevent pressure points.
Consistent repositioning, combined with proper support surfaces, helps maintain skin integrity and comfort while reducing the risk of sores.
Monitoring Skin Condition and Identifying Risks
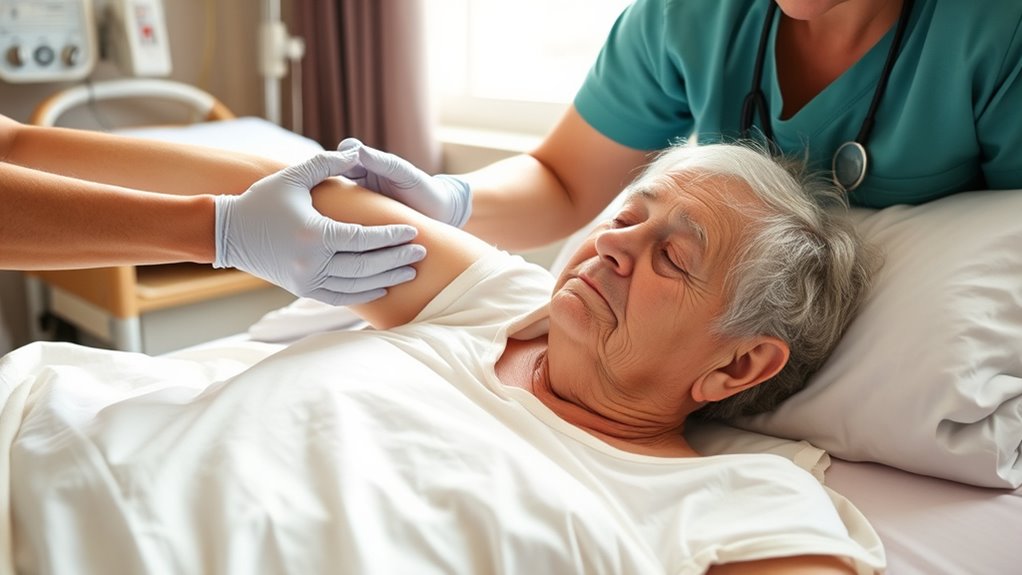
Regularly monitoring the skin condition of bedbound seniors helps catch early signs of pressure damage before they develop into serious ulcers. Check the skin at high-risk areas like the sacrum, heels, elbows, and hips daily, looking for redness, discoloration, or warmth. Use your hands to gently feel for swelling or abnormal textures, which may indicate developing tissue issues. Keep an eye out for skin that feels shiny, thin, or broken, as these are signs of compromised integrity. Document any changes you observe and report persistent redness or skin breakdown immediately. Regular assessments allow you to adjust repositioning schedules, support surfaces, or skin care routines promptly. Staying vigilant helps prevent minor issues from progressing into severe pressure ulcers, ensuring your senior’s comfort and health.
Special Considerations for Fragile Skin and High-Risk Areas

Fragile skin requires extra care during repositioning because it can tear or bruise easily, increasing the risk of pressure wounds. You must be gentle and attentive to high-risk areas. To protect these vulnerable spots:
- Use soft, padded supports or specialty cushions to reduce pressure on delicate regions like the sacrum, heels, and elbows.
- Avoid pulling or dragging the skin; instead, lift and shift slowly using proper techniques.
- Regularly inspect high-risk zones for redness, skin thinning, or tears, and document any changes immediately.
Additionally, keep skin moisturized with gentle products and ensure bedding is smooth and wrinkle-free to prevent friction. These steps help minimize trauma and support skin integrity in seniors with fragile skin.
Incorporating Mobility and Nutrition Into Care

Incorporating mobility and nutrition into care is essential for maintaining skin integrity, preventing complications, and promoting overall well-being in bedbound seniors. Encouraging gentle movements, like passive limb exercises or repositioning, boosts circulation and reduces pressure buildup. Even small, frequent movements help prevent muscle atrophy and improve comfort. Proper nutrition, especially adequate protein intake, supports skin repair and immune function, making tissues more resilient. Ensuring hydration also maintains skin elasticity. Collaborate with dietitians to develop individualized meal plans that meet nutritional needs. Regularly assess skin condition and adjust mobility activities accordingly. Combining movement and nutrition creates a holistic approach that supports tissue health, reduces ulcer risk, and enhances your senior’s overall quality of life.
Collaborating With a Multidisciplinary Team

Effective repositioning of a bedbound senior often requires input from a team of healthcare professionals. You’ll benefit from their combined expertise to develop a personalized care plan. To maximize effectiveness, consider these key steps:
- Coordinate with nurses and wound care specialists to identify pressure points and determine ideal repositioning schedules.
- Work with physical and occupational therapists to incorporate mobility strategies that support skin health and circulation.
- Consult dietitians to ensure proper nutrition, especially protein intake, to promote skin healing and tissue integrity.
Frequently Asked Questions
How Can I Safely Reposition a Senior With Limited Strength or Mobility?
To safely reposition a senior with limited strength or mobility, use proper lifting techniques and equipment like slide sheets or transfer devices. Communicate clearly throughout, and work with others if needed to avoid strain. Protect fragile skin by using pillows, foam wedges, and cushions to offload pressure points. Move slowly and gently, ensuring their comfort and safety, and check skin afterward for any signs of redness or irritation.
What Signs Indicate a Developing Pressure Sore Before Visible Skin Damage?
You should watch for signs like persistent redness that doesn’t fade, warmth or swelling, and skin that feels firm or tender to touch. Also, look for darkened skin or blisters, which can indicate tissue damage starting beneath the surface. If you notice these changes, it’s a clear sign to reposition immediately, as early detection helps prevent full-blown sores and promotes healing.
How Do I Adjust Repositioning Frequency for Seniors With Fragile Skin?
You should increase repositioning frequency for seniors with fragile skin, moving them every 1 to 2 hours instead of the usual 2-hour interval. Regularly check their skin for signs of redness or irritation, and use specialized support surfaces like pressure-relieving mattresses and cushions. Be gentle during repositioning, ensuring proper padding, and avoid shear forces. Close monitoring and tailored schedules help minimize skin breakdown risks for delicate skin.
What Are Effective Methods to Offload Pressure From the Sacrum and Heels?
Think of your senior’s skin as a delicate garden needing protection. To offload pressure from the sacrum and heels, elevate the hips to a 30-degree lateral tilt and use pillows or foam wedges under the sacrum and heels. Suspend heels off the bed using heel protectors, and rotate positions regularly. These methods create safe zones, allowing tissues to breathe and recover, much like tending to fragile plants carefully.
How Can Caregivers Prevent Shear Injuries During Repositioning?
You can prevent shear injuries by using proper repositioning techniques, such as scooping with sheets instead of dragging the patient. Always lift or slide the person gently, avoiding friction against the skin. Check for skin integrity after repositioning, and make certain the patient is well-supported with pillows or foam wedges to reduce shear forces. Communicate clearly, move smoothly, and never force changes to minimize skin damage risks.
Conclusion
By understanding the importance of repositioning, establishing a routine, and using proper techniques, you can effectively prevent sores. Selecting supportive surfaces, monitoring skin, and considering special needs are all essential steps. Incorporating mobility, nutrition, and teamwork into your care creates an extensive approach. When you stay consistent, attentive, and proactive, you not only protect their skin but also enhance their comfort, dignity, and quality of life. Your dedication makes all the difference.