To prevent bedsores in bedridden seniors, you should regularly turn them every two hours and use pressure-relieving support surfaces like foam mattresses or alternating pressure overlays. Keep their skin clean, dry, and well-moisturized, and check for early signs of skin changes daily. Proper transfer techniques reduce friction and shear forces. Ensuring good nutrition and hydration also helps. If you’re interested in learning more about effective strategies, keep exploring proven prevention methods.
Key Takeaways
- Reposition bedridden seniors every 2 hours to relieve pressure and promote circulation.
- Use pressure-relieving mattresses and support surfaces like foam or alternating pressure air beds.
- Keep skin dry and clean, applying barrier creams to prevent moisture-related skin breakdown.
- Minimize friction and shear during transfers with proper techniques and supportive devices.
- Regularly inspect skin for early signs of pressure ulcers and adjust care plans promptly.

Skechers Women's Hands Free Slip-Ins Go Walk Flex-Relish Sneaker, Black/Black, 9.5 Wide
EFFORTLESS SLIP-ON DESIGN: These slip on shoes for women feature a convenient laceless design with breathable athletic mesh...
As an affiliate, we earn on qualifying purchases.
Understanding the Risks Faced by Bedridden Elderly Individuals

Understanding the risks faced by bedridden elderly individuals is essential for effective prevention. As someone caring for an aging loved one, you should recognize that their vulnerability increases with age-related changes. Loss of subcutaneous fat, thinning skin, and decreased blood flow make their skin more prone to damage. Prolonged immobility further heightens the risk, as constant pressure on bony prominences can cause skin breakdown in as little as 12 hours. Additionally, intrinsic factors like arthritis or paralysis reduce their ability to shift weight naturally. External factors, such as contact with hard surfaces or moisture from incontinence, also contribute. Being aware of these risk factors helps you implement timely interventions, ensuring better skin integrity and preventing pressure ulcers before they develop. Recognizing the importance of pressure redistribution can significantly aid in reducing skin damage and promoting comfort in bedridden seniors. Proper pressure management techniques are crucial in minimizing the risk of skin breakdown and supporting overall comfort. Incorporating herbal remedies, such as soothing herbal-infused skin treatments, may also help maintain skin health and resilience. For example, moisturizing the skin regularly can improve skin elasticity and reduce cracking, further preventing breakdown. Implementing regular repositioning strategies and using appropriate support surfaces can further enhance skin protection and healing.

Hike Footwear HF Stride – Hands-Off & Ergonomic Barefoot Shoes, Thin Sole & Ultra-Light, Effortless Wear Unisex Dark Gray
🔹 Size Recommendation: For optimal comfort and fit, we recommend ordering one size larger than your usual size,...
As an affiliate, we earn on qualifying purchases.
Recognizing Key Factors Contributing to Pressure Ulcer Development

You need to understand how prolonged pressure on bony areas can quickly cause skin damage, especially when repositioning isn’t frequent enough. Moisture from incontinence or sweat weakens the skin, making it more vulnerable to breakdown. Friction and shear forces from transfers or movements can also harm the skin, increasing the risk of pressure ulcers. Additionally, inadequate assessment and proper care planning can leave at-risk seniors more susceptible to developing bedsores. Regularly monitoring skin integrity and recognizing early signs of tissue damage are essential components of effective pressure ulcer prevention strategies. Being aware of pressure distribution and ensuring proper support surfaces can significantly reduce the risk of developing these injuries.
Prolonged Pressure Impact
Prolonged pressure on the skin, especially over bony prominences, is a primary factor in pressure ulcer development. When you stay in one position too long, the continuous pressure cuts off blood flow, depriving tissues of oxygen and nutrients. Over time, this causes cell death and skin breakdown. To prevent this, it’s essential to understand how pressure builds and affects vulnerable areas. Free Floating techniques can help distribute pressure more evenly across the body, reducing the risk of ulcers. Understanding pressure distribution is vital for implementing effective repositioning strategies. Additionally, using specialized support surfaces can help alleviate pressure and protect at-risk areas. Bony areas like hips, heels, and sacrum bear the brunt of sustained pressure. High pressure impairs blood circulation, leading to tissue ischemia. Longer pressure duration increases ulcer risk considerably. Lack of movement allows pressure to remain constant. Proper repositioning relieves pressure, reducing tissue damage. Recognizing how pressure buildup occurs emphasizes the importance of regular movement in prevention. Incorporating airflow around the body and ensuring proper positioning can further improve tissue perfusion.
Skin Moisture Effects
Moisture from incontinence, perspiration, and wound drainage considerably weakens the skin’s integrity, making it more vulnerable to pressure-related injuries. When skin stays damp, its outer layers soften and become prone to breakdown. Excess moisture also promotes bacterial growth, increasing infection risk and delaying healing. If you don’t manage moisture effectively, the skin’s protective barrier deteriorates faster, especially over bony prominences. Regularly check for dampness and promptly dry and clean the skin. Using moisture-wicking dressings and barrier creams helps create a protective layer. Proper moisture management techniques minimize skin maceration and preserve skin strength. Additionally, understanding common financial terms related to healthcare costs can help families plan for potential expenses associated with wound care. Recognizing skin integrity factors can further aid in developing comprehensive skin protection strategies. Implementing moisture control techniques can significantly reduce the risk of skin breakdown. Incorporating preventive measures, such as repositioning and pressure relief, enhances overall skin health and reduces the likelihood of pressure ulcers.
Friction and Shear
How do friction and shear forces contribute to pressure ulcer development? Friction occurs when your senior’s skin rubs against bedding or clothing, causing surface damage. Shear happens when underlying tissues slide against bones during movements or repositioning, damaging blood vessels and impairing circulation. These forces weaken the skin’s integrity, making it more vulnerable to breakdown. To prevent this, avoid dragging patients during transfers, use proper support surfaces, and reposition carefully. Additionally, understanding skin fragility can help in selecting appropriate interventions to protect vulnerable areas. Recognizing the role of pressure distribution is also essential in minimizing localized stress on the skin and tissues. Proper management of support surfaces can significantly reduce the risk of pressure ulcers by evenly distributing pressure and minimizing shear forces. Incorporating pressure relief techniques can further enhance protection by reducing sustained pressure on vulnerable regions.

Scurtain Mens Walking Shoes Wide Width Diabetic Shoes for Men Elderly Seniors Adjustable Swollen Feet Neuropathy Orthopedic Edema Shoes Breathable Barefoot Zero Drop Sneakers Size 10 Black
〓 Comfy wide width Shoes: Designed with upgraded wide toe box, these barefoot-inspired shoes keep your toes in...
As an affiliate, we earn on qualifying purchases.
The Importance of Regular Repositioning and Turn Scheduling

You need to follow established guidelines for repositioning your loved one, typically every two hours, to prevent pressure sores. The type of mattress also makes a difference, with foam mattresses reducing pressure more effectively than standard ones. Additionally, timing your turns appropriately—such as every 30 minutes for wheelchair users—can markedly decrease the risk of skin breakdown. Ensuring proper pressure redistribution through appropriate positioning and support surfaces is essential for skin health. Proper pressure distribution can be achieved with specialized cushions and positioning devices that help minimize prolonged pressure on vulnerable areas. Using ventilation considerations can also improve overall skin condition by reducing moisture buildup and promoting healing.
Repositioning Frequency Guidelines
Repositioning your bedridden patients at regular intervals is essential for preventing pressure ulcers. The recommended schedule is every two hours, as this minimizes prolonged pressure on vulnerable areas. For wheelchair-bound patients, repositioning every 30 minutes helps maintain blood flow and reduces shear and friction risks. Consistent turns prevent tissue ischemia, especially over bony prominences. Using supportive surfaces like foam mattresses can extend safe intervals, but schedules should still follow guidelines. Remember, longer intervals on high-quality surfaces can be effective, but not for all patients. Regular repositioning guarantees skin integrity, reduces moisture buildup, and supports circulation.
- Promotes consistent blood flow and oxygen delivery
- Reduces risk of moisture accumulation and skin maceration
- Prevents friction and shear forces during transfers
- Enhances overall comfort and dignity
- Supports early detection of skin issues
Impact of Mattress Type
Selecting the right mattress type plays a crucial role in preventing pressure ulcers, especially when combined with proper turn scheduling. Foam mattresses, for example, reduce pressure by 20-30%, offering better pressure redistribution than standard beds. Advanced support surfaces like alternating pressure air mattresses (APAM) and pressure-reducing mattresses further enhance protection by evenly distributing weight and minimizing pressure points. These specialized mattresses can appreciably lower the risk of skin breakdown, especially for those with limited movement. When paired with regular repositioning, the right mattress helps maintain blood flow and reduces friction and shear forces on vulnerable areas. Choosing the appropriate mattress based on your loved one’s needs supports skin integrity and complements your efforts to prevent bedsores effectively.
Optimal Turn Timing
Regular repositioning is essential in preventing pressure ulcers among bedridden seniors, as prolonged pressure on bony prominences can cause skin breakdown in as little as 12 hours. Proper turn timing guarantees blood flow and reduces shear forces that damage tissue. You should reposition patients every two hours to maintain skin integrity, following established guidelines. Using advanced support surfaces can extend safe sitting times but doesn’t replace scheduled turns. Keep in mind:
- Consistent schedules prevent unintentional neglect of repositioning
- Monitoring skin condition helps identify early signs of pressure damage
- Using supportive devices enhances the effectiveness of turns
- Careful documentation ensures adherence and allows adjustments
- Individual patient needs may require tailored turn intervals
Sticking to ideal timing minimizes ulcer risk and promotes healthier skin.

Spesoul Wide Womens Walking Shoes Adjustable Diabetic Shoes Breathable Zero Drop Barefoot Shoe Neuropathy Edema Nursing Shoe Wide Width Sneakers 8.5 Navy
Wide Width:these wide womens walking shoes have a wide toe box design,allowing the feet to stay their natural...
As an affiliate, we earn on qualifying purchases.
Selecting Effective Support Surfaces and Pressure-Relief Devices
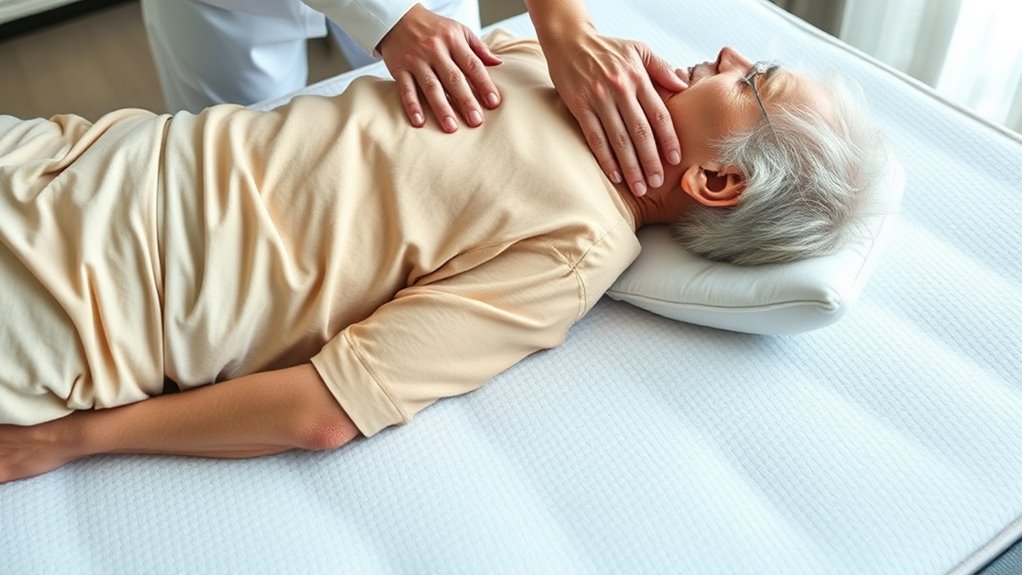
Choosing the right support surfaces and pressure-relief devices is essential for effectively preventing pressure ulcers in bedridden seniors. You should select mattresses that distribute pressure evenly, such as foam or alternating pressure air mattresses, to reduce sustained pressure on bony prominences. Overlay cushions, heel protectors, and specialized wheelchair cushions help further minimize localized pressure and shear forces. It’s important to match device types to each patient’s needs, considering factors like skin condition, mobility level, and comfort. Using pressure-relief devices in combination with proper repositioning schedules maximizes protection. Regular assessment ensures devices continue to meet the patient’s needs and prevent skin breakdown. Investing in appropriate support surfaces can considerably lower the risk of ulcer development and improve overall comfort.
Implementing Predictive Nursing Strategies for Prevention

Implementing predictive nursing strategies plays a crucial role in preventing pressure ulcers among bedridden seniors by proactively identifying those at high risk. You analyze patient data, monitor skin integrity, and assess mobility to anticipate potential issues before they develop. This approach allows you to tailor interventions, optimize repositioning schedules, and adjust pressure-relief devices effectively. By focusing on early detection, you reduce the likelihood of ulcer formation and improve outcomes.
- Regularly evaluate skin condition and mobility status
- Use risk assessment tools to identify vulnerable areas
- Educate caregivers on early warning signs and preventive actions
- Collaborate with multidisciplinary teams for personalized care plans
- Adjust pressure-relief devices based on ongoing assessments
Utilizing Evidence-Based Practices for Pressure Ulcer Prevention

Utilizing evidence-based practices is essential for effectively preventing pressure ulcers in bedridden seniors. You should regularly assess each patient’s risk using tools like the Braden Scale, but remember these tools are guides, not guarantees. Educate caregivers on proper repositioning techniques, skin inspections, and device use to catch early signs of breakdown. Keep head-of-bed elevation at or below 30 degrees to reduce shear forces. Confirm skin stays dry and moisturized, and promote adequate nutrition to support tissue integrity. Use pressure-relieving mattresses and cushions tailored to individual needs, combining them with scheduled repositioning. Active, anticipatory nursing care that incorporates these proven strategies can notably lower ulcer risk, improve outcomes, and enhance patient comfort. Consistent application of these practices makes a tangible difference.
Optimizing Nutrition and Skin Care for Vulnerable Seniors
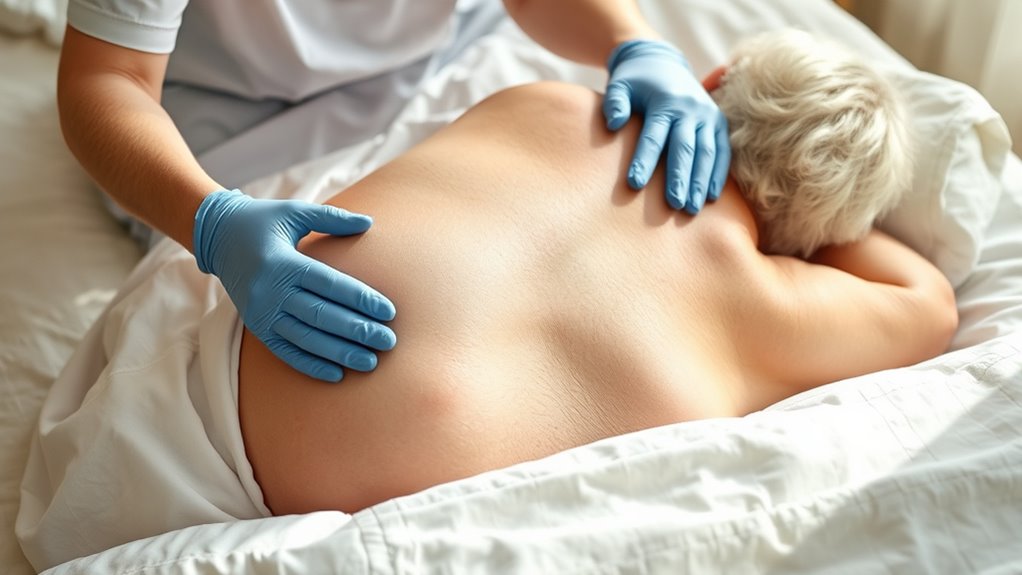
Effective pressure ulcer prevention depends not only on proper repositioning and device use but also on optimizing nutrition and skin care. You should guarantee your senior’s diet provides adequate protein, vitamins, and minerals to support skin integrity and wound healing. Hydration is equally crucial, as dry skin is more prone to breakdown. Regularly inspect the skin for early signs of damage, and keep it clean and dry. Use gentle cleansers and moisturizers suited for sensitive skin to prevent dryness and irritation. Incorporate these strategies:
- Provide balanced, protein-rich meals to promote tissue repair
- Maintain adequate hydration to keep skin supple
- Use skin-friendly cleansers and emollients
- Encourage frequent skin checks for early issues
- Avoid harsh soaps and abrasive products that damage delicate skin
Managing Moisture and Minimizing Friction and Shear Forces

You can reduce the risk of bedsores by effectively managing moisture from incontinence and perspiration, which weakens skin. Using absorbent pads and maintaining skin dryness helps prevent breakdown. Additionally, minimizing friction and shear forces during repositioning protects fragile skin from unnecessary damage.
Moisture Control Strategies
Moisture management is essential in preventing pressure ulcers among bedridden seniors because excess moisture weakens the skin’s integrity and increases the risk of breakdown. To control moisture, regularly check for incontinence, perspiration, or wound drainage, and promptly address these issues. Use absorbent pads or barrier creams to protect the skin from moisture exposure. Keep the skin clean and dry, especially around bony prominences. Proper positioning prevents prolonged moisture contact and reduces friction. Ensure the environment is well-ventilated to decrease sweating.
- Use barrier creams to protect skin from moisture.
- Change incontinence pads frequently to prevent dampness.
- Keep linens dry and clean to avoid bacterial growth.
- Promote good hygiene for skin health.
- Monitor for signs of excessive moisture and adjust care accordingly.
Friction Reduction Techniques
Friction and shear forces considerably contribute to skin breakdown in bedridden seniors, especially when moisture is present. To minimize these forces, start by ensuring your patient’s skin stays dry and clean, reducing the risk of moisture-related damage. Use smooth, gentle transfer techniques to move or reposition your patient, avoiding dragging or pulling on the skin. Employ supportive devices like slide sheets or transfer boards to reduce friction during repositioning. Adjust bed surfaces with pressure-relieving mattresses that cushion the skin and distribute pressure evenly. When turning or repositioning, lift rather than drag the patient, and encourage proper hydration and skin care to maintain skin integrity. Combining these techniques helps prevent unnecessary friction and shear, protecting vulnerable skin areas from breakdown.
Shear Force Prevention
Proper management of moisture and careful control of shear forces are essential in preventing skin damage in bedridden seniors. Excess moisture weakens the skin, making it more vulnerable to shear injuries. Shear occurs when skin layers slide against each other or surfaces, damaging blood vessels and tissue. To minimize these risks, use moisture-wicking materials and keep the skin dry. Position your patient carefully to avoid dragging or pulling during transfers. Reposition them regularly, especially when changing their angle or position. Employ pressure-relief devices that reduce friction and shear. Ensure the head of the bed stays below 30 degrees to prevent sliding and shear forces.
- Use supportive surfaces that decrease skin friction
- Avoid dragging during repositioning
- Keep skin dry with proper moisture management
- Reposition frequently to prevent prolonged shear
- Use cushions and overlays to distribute pressure
Educating Caregivers and Family Members on Prevention Techniques

Educating caregivers and family members is vital for preventing bedsores in bedridden seniors, as they play a key role in daily skin care, repositioning, and environmental management. You should learn to inspect the skin regularly, especially over bony prominences, for early signs of redness or breakdown. Reposition the senior at least every two hours to relieve pressure and improve circulation. Use proper techniques during transfers to reduce friction and shear forces. Ensure the bedding is clean, dry, and soft, and consider pressure-relief devices if recommended. Maintain good nutrition and hydration, as these support skin health. Educate yourself on risk factors and intervention strategies, and communicate with healthcare providers for tailored advice. Your proactive involvement greatly reduces the risk of pressure ulcers and promotes comfort and healing.
Monitoring and Early Detection of Skin Changes in Bedridden Patients

Regular monitoring of your bedridden patient’s skin is essential because early detection of skin changes can prevent the development of pressure ulcers. You should inspect their skin daily, focusing on bony prominences like hips, heels, and sacrum. Look for redness, discoloration, warmth, swelling, or any broken skin. Keep an eye on moisture levels from incontinence or sweating, which can weaken skin integrity. Use proper lighting and gentle handling to avoid causing friction or shear. Document any skin changes and notify healthcare providers immediately for prompt intervention. Remember, timely action can halt progression before ulcers form.
- Recognize early signs like redness or warmth, not just open wounds
- Check skin in hidden areas and skin folds regularly
- Keep skin dry and clean to minimize irritation
- Use mirrors or ask for assistance for hard-to-see spots
- Educate caregivers on consistent skin assessment techniques
Frequently Asked Questions
How Can I Tell if a Pressure Ulcer Is Starting to Develop?
You can tell a pressure ulcer is starting to develop if you notice redness that doesn’t fade after pressure is relieved, especially over bony areas like hips or heels. Look for skin that feels warm, firm, or swollen. In early stages, there might be a shiny or discolored spot. Keep an eye out for pain or tenderness, and check regularly, especially in high-risk areas, to catch problems early.
Are There Specific Foods That Help Prevent Bedsores?
Think of your skin as a fortress that needs strong building blocks. Foods rich in protein, like lean meats and beans, help repair and strengthen skin tissue, reducing bedsores risk. Vitamin C from citrus fruits boosts collagen production, promoting healthy skin. Zinc-rich foods like nuts and seafood support healing. Eating a balanced diet with these essentials acts like a shield, keeping the skin resilient and less prone to breakdown.
What Are the Best Positions to Reduce Pressure on Bony Prominences?
You should position the patient to minimize pressure on bony prominences like the sacrum, heels, and hips. Reposition every two hours, shifting slightly to avoid prolonged pressure. Use pillows or foam wedges to offload pressure points and elevate the head no more than 30 degrees to reduce shear forces. Keep the skin dry and well-supported, and consider specialized support surfaces to help distribute weight evenly.
How Do I Choose the Right Pressure-Relief Device for My Loved One?
Selecting the appropriate pressure-relief device is akin to discovering the ideal shoe for comfort—you want it to fit your loved one’s needs. Begin by assessing their risk factors, mobility level, and skin condition. Consult with a healthcare professional to choose from foam, gel, or air mattresses, as studies demonstrate tailored devices considerably reduce pressure points. Regularly evaluate comfort and effectiveness to guarantee ideal pressure redistribution and prevent skin breakdown.
When Should I Seek Professional Help for Skin Changes or Early Wounds?
You should seek professional help as soon as you notice skin changes like redness, discoloration, or warmth, even if there’s no open wound. If you see early wounds, blisters, or skin breakdown, contact a healthcare provider immediately. Prompt evaluation guarantees proper treatment and prevents worsening. Don’t wait or try to treat it yourself—early intervention is key to avoiding serious complications and promoting healing.
Conclusion
By staying proactive and attentive, you can turn the tide against bedsores before they take hold. Regular repositioning, proper skin care, and understanding risk factors are your armor in this fight. Think of it as tending a delicate garden—consistent care keeps it healthy and thriving. With your dedication, you guarantee your loved one’s comfort and dignity, transforming what seems like a formidable challenge into a manageable task.








